It’s never pleasant as a parent when your child comes down with something. You put plans on hold, you schedule plenty of rest, you try to keep everything as clean as possible so no one else gets sick. You grieve for your child when they have to miss out on something they love; you soothe their fevers and pull their hair back when they vomit and reassure them with your presence; you watch their symptoms accumulate and decide whether to wait it out at home or call the doctor. But it’s mostly routine by the time you have three kids and the oldest is six – you’ve seen a lot of winter colds and coughs and stomach bugs by then.
It’s a bit different when all around you society is panicking about a virus whose symptoms just so happen to match your child’s. When you know enough about virology and epidemiology to understand the public health risks that make complacency the greater danger to the wider community, and don’t want to become an epicenter for a new wave of outbreaks. When you’ve heard an experienced doctor comment on how suddenly COVID-19 patients can go from stable on oxygen to needing mechanical ventilation. When you’re considered essential personnel in a lab on a campus that has already had 15 confirmed COVID-19 cases – despite serious testing delays and shortages – and when your child’s grandmother spent time with them after visiting Seattle in the early stages of the outbreak when more people were still skeptical.
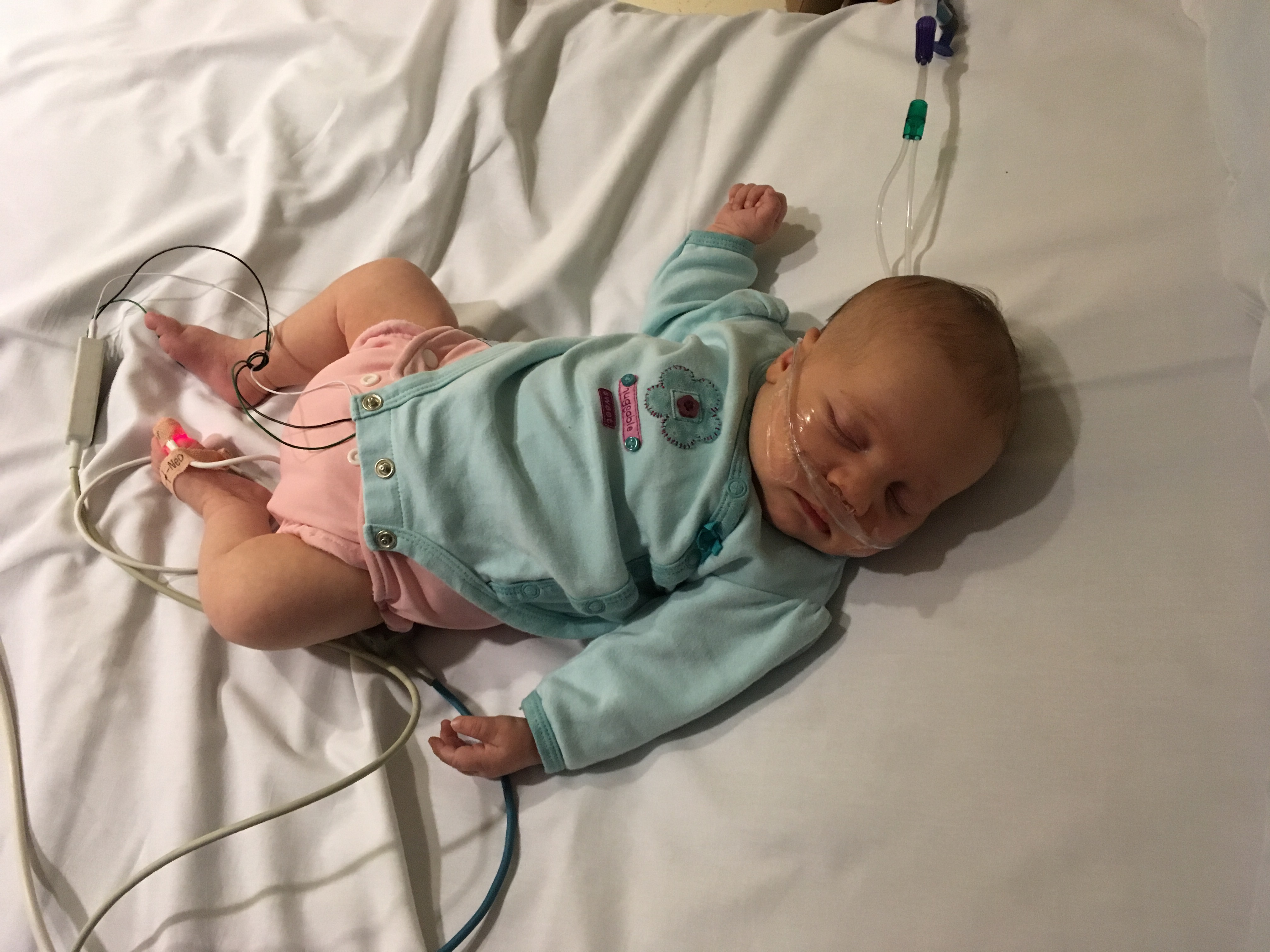
It’s an eagle eye on your child’s breathing, then: an ear to his chest for wheezing, a glance around his collarbone and ribs for retractions, a counting with a stopwatch while he sleeps and the breaths come fast even though he’s at rest. It’s pulling out the nebulizer and albuterol to see if it makes a difference, and planning to go to urgent care if it doesn’t. It’s taking your child’s temperature multiple times a day even though the quick kid-friendly one is dead and you have to sit holding the old thermometer in place for three minutes waiting for a result. It’s making sure he covers when he coughs and that his siblings are washing their hands before every meal and after every time using the shared bathroom.
It’s a long and almost teary conversation with the nurse on the other end of the insurance-provided triage line (I love those nurses – they have helped me through so much anxiety and given me so much solid guidance when I’m not sure what to do), then, going through symptoms and addressing concerns. It’s a drop of the stomach when the nurse practitioner at the ER tells you your child’s symptoms are concerning she’s going to call the COVID-19 hotline to get you the best plan of action. It’s a panic that won’t let you sleep when she tells you that if his symptoms get worse – if he stops responding to the albuterol before four hours have passed and he can have another dose (the thing that triggered the original urgent care visit, so a very possible event), to be precise – he should go to the ER immediately, with a mask on, and you should alert the ER staff of the possibility of the coronavirus.
With the morning will come more things you can do, again, practically and tangibly for your child: antibiotics for an ear infection, albuterol for a cough, tylenol for a fever, hugs and kisses and books and simple foods to soothe a sick but hungry stomach, appointments to make for lab work. You can be with him again, in the light of day, to watch his energy levels and breathing. But in the night, when you both need to sleep, there is nothing to do except pray. And the prayer that seems to me most fitting, when there is fear and a valid reason to fear and your child whom you love is sleeping fitfully across the hall, is the antiphon to the canticle of Simon sung in Evening Prayer:
Protect us, Lord, as we stay awake; watch over us as we sleep, that awake, we may keep watch with Christ, and asleep, rest in His peace.

 The book is primarily about public health policy, and explains quite a bit about both the history of dentistry and the current state of dental health access and expense. But it covers this potentially dry topic in a manner that is both rationally and emotionally powerful, drawing the reader in through stories of individuals affected by societal pressure for “perfect” teeth or by societal neglect of oral health. Before reading this, I had never realized the extent of either the available cosmetic dentistry services or the overall risks of poor dental health (I guess I live in a comfortable middle-class bubble here…), and I was surprised and saddened by much of what I learned. This book does not engage in a lot of philosophizing; it accumulates stories and statistics and allows the reader to come to their own conclusions.
The book is primarily about public health policy, and explains quite a bit about both the history of dentistry and the current state of dental health access and expense. But it covers this potentially dry topic in a manner that is both rationally and emotionally powerful, drawing the reader in through stories of individuals affected by societal pressure for “perfect” teeth or by societal neglect of oral health. Before reading this, I had never realized the extent of either the available cosmetic dentistry services or the overall risks of poor dental health (I guess I live in a comfortable middle-class bubble here…), and I was surprised and saddened by much of what I learned. This book does not engage in a lot of philosophizing; it accumulates stories and statistics and allows the reader to come to their own conclusions.